Lean and Kaizen in Healthcare
My most recent post about Lean in Japan and in Japanese hospitals has been a popular one and has generated many comments on social media and on the post itself.
As I wrote in that post, learning more about how Japanese hospitals and healthcare organizations practice, or don’t practice, what we call “Lean” in the West has been one of my top interests since moving to Japan 14 months ago.
Gemba visits and discussions with senior leaders
I’ve had the fortune of being able to talk with senior leaders of many Japanese hospitals known for their kaizen and quality improvement practices – either coupled with a gemba visit or at a kaizen-focused healthcare conference in Japan.
I am tremendously grateful for the time all of these hospital leaders have given me and for their openness in sharing their approaches to quality, continuous improvement and kaizen.
In the past two weeks I had the opportunity to visit two hospitals in Tokyo: a community hospital known for its approach to quality improvement and follow-up conversations with a large international hospital that I have previously written about.
These visits and conversations has all influenced my thinking about Lean practices in Japan and were the catalyst for writing my most recent blog post.
Tokyo Hospital’s approach to Medical Quality Improvement

This post is about my visit to a Tokyo hospital that calls its approach to kaizen”Medical Quality Improvement” (MQI). Nerima General Hospital is located in the northwest area of Tokyo.
Thank you to Mark Graban who connected me with Nerima’s CEO, Dr. Shuhei Iida. I emailed him directly and he and the Medical Director of MQI were generous to schedule a private meeting with me.
Mark has also written about his experience visiting Nerima General and his reflections on Lean in Japan and in Japanese hospitals.
Personal discussions with CEO and Medical Director of MQI
I am appreciative that the CEO and Medical Director of MQI met with me for over 90 minutes and shared their personal and organizational approaches to quality improvement.
Both physician leaders speak very good English, although we did not have an interpreter, so there were times that our conversation didn’t go as in-depth as it might have otherwise. I’m continually impressed by the level of English fluency of so many Japanese leaders and physicians that I have met (granted, those who are able to speak English are probably more likely to respond to my requests!).
During our engaging discussion, they both jumped up to a whiteboard multiple times to map out their ideas and thoughts. Following our talk in the conference room, the MQI Director gave me a tour of the nursing wards, surgery center, lab, radiology and other areas.
20 years of Medical Quality Improvement and teaching MQI

The 20th anniversary of MQI passed just a few months ago and they have published a book to commemorate its achievements and lessons. My hosts showed me the book, which included photos of many of the MQI teams that have conducted improvement project.
Dr. Iida is clearly passionate about quality and MQI. He knows that leadership starts at the top.
He is also a great supporter of developing people, as evidenced by the multiple books he has written about improvement methodologies. His goal through writing the books (some of these co-authored with the Medical Director) is to give more people knowledge of process improvement as applied to healthcare. Topics for the books include: work flow charts, Failure Mode Effect Analysis (FMEA), and Root Cause Analysis (RCA).
The origins of Medical Quality Improvement
Dr. Iida said that five years after he became CEO, he realized that the hospital needed a different approach to quality. But instead of telling his senior management team that a better approach was needed, he supplied them with books on quality management.
In 1996, Dr. Iida took his team on what turned out to be a seminal retreat at an onsen (Japanese hot spring) where the team decided the hospital would start using Total Quality Management, which they rebranded as “Medical Quality Improvement”.
The first Medical Director of MQI was part of this initial trip to the onsen and served for almost a decade. The Director that I met is an internal medicine specialist. He is the second Medical Director of MQI and has been in this role since 2005.
Nemawashi: plant the seeds and be patient for them to grow
Dr. Iida wisely shared with me that “it was their own idea. I didn’t say anything.” As Isao Yoshino has said many times to me, it is better to show than to tell!
I commented that this approach was Dr. Iida’s “nemawashi” for MQI. They both laughed and agreed!
I was taught many years ago that “nemawashi” is a Japanese word that means “tilling the soil” and laying the groundwork for a new idea to take root. It is one of the Japanese words, like “gemba”, that have made their way into English Lean terminology as we don’t have a word that quite expresses the same meaning.
Patience and tenacity are two Japanese cultural qualities, which are vital to “nemawashi”, as I wrote in the comments on my previous post, that help facilitate successful Lean practices in Japan.
Side note on gender roles and where decisions are made
Side note: Gender roles globally have always been a topic of interest for me, and especially here in Japan where the gender divide is great. A lot of Japanese business and discussion happens informally – including at the onsen while naked. This works when everyone is male, as it was in this case (and as most in Japan still).
I am curious to how this practice of having important discussions – at the onsen or late at night after work – will need to adjust if Japan is desirous to achieve Prime Minister Abe’s goal of 30% women in management positions by 2020? You can read more about my observations and thoughts about gender roles in Japan (and elsewhere).
MQI Annual Projects
Quality improvement at Nerima is mainly done via improvement teams that conduct year-long projects, as it is at the two other hospitals I’ve visited in Japan – St. Luke’s and Iizuka.
Every year the Nerima senior management team chooses a “unifying them” that all MQI projects must fit into. You can see a good explanation of Nerima’s MQI process and the unifying themes from the past 20 years on Nermia’s website (turn on Google translate to be able to read it in your language).
About ten years ago they started their current approach to annual team-based projects. Starting in April of each year, the hospital leadership nominates about 40 staff and physicians to participate in MQI projects. They form eight to teams teams consisting of four to five people each.
Dr. Iida outlined four rules for MQI teams:
- Teams will be cross-functional: team members should come from at least four different areas or departments
- Physicians will be involved: each team must include at least one doctor
- Teams will choose their own topic or theme for their improvement project (he called this “free topic”)
- Each team must choose a difficult goal (Dr. Iida reserves the right to challenge a team if their target is not challenging enough).
The teams work together over the course of eight months on their improvement project, which culminates in an event in December where the teams share what they accomplished to the rest of the hospital and outside guests.
Engaging everyone?
I asked how the hospital engages frontline staff in MQI, kaizen and continuous improvement. They said that anyone can participate in a MQI annual project and that they can take classes to learn about quality improvement methodologies.
The MQI Medical Director shared that it can be hard to get physicians involved and part of his role is to persuade his colleagues to participate in one of the improvement teams.
MQI Department
I asked the Medical Director about his department. He said that in addition to himself, there are 10 staff. Their role is to facilitate the MQI projects and help the teams. They are skilled in PDCA cycles and being able to negotiate issues between different departments. Sounds familiar from my previous similar roles in hospitals in the United States!
Policy deployment for 2016
The senior management team also chooses five topics (or “policies” in Japanese) that are the focus of the year. One might think of this as as “policy deployment” or “strategy deployment”, though I didn’t get to learn how the policies are deployed down to the frontline beyond leadership sharing the topics and posting them broadly.
Dr. Iida showed me a piece of A4 paper on the wall that had the policies (goal) areas for 2016 printed on in. He translated the policies for me and shared what they mean to him in more detail. I took a picture (with permission) and my Japanese teacher also helped further translate what was written (see below).
Hospital goals for 2016
The overall aim of the year is “to do medical care and management that can be dependable, be reliable, and be something to be proud of”. (Mark Graban also wrote about the theme and aim of the year for when he visited in his blog post about this hospital).
Dr. Iida noted that the first three goals were borrowed from General Electric.

The five policies for 2016 are:
- “Boundarylessness” – “note just pull down the boundary but to cooperate organically” (I suggested that the term “boundarylessness” would commonly be known as “breaking down the silos”)
- “Stretch” – “clearly understand one’s role, but also go beyond your role.”
- “Speed” – “‘NOW’ is important'”
- “MQI Squared” – “reconstruct MQI and make the MQI action go smoothly” (in other words – improve the actual MQI process of improvement)
- “Be a process owner” – “control the operation (self-center)”
It is this last point of being a process owner and being “self-centered” that Dr. Iida spent a lot of time talking about during our meeting.
Self-centered, not patient-centered
Dr. Iida shared his philosophy that healthcare should not be seen as “patient centered”, but rather as “self centered”. He showed me a Venn diagram in one of his books that is comprised of four circles. He shared that the four concepts were: Environment, Other People, System Application, and Facility – with the self (individual) at the center.
He believes that it is each of our jobs to provide patient-centered care, and that we must do it for ourselves, not for the patients.
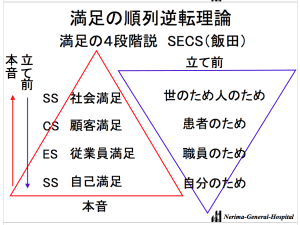
He described that we typically of doing something for society –> customers –> employees –> self. But, as shown in the image to the left, he thinks we should flip this pyramid on its head and have the self be the driving reason (self –> employees –> customers –> society). I wish I could read more Japanese so that I could further explore these concepts, which are laid out in his books.
Delivering quality healthcare, should be our job and should start with each of us. He pointed to himself multiple times while describing his philosophy – emphasizing that it is HIS job as the CEO to deliver quality care.
This is aligned with the Lean philosophy of people development.
You can read more about Dr. Iida’s approach in an interview translated to English from 2001 and from an article that he wrote (though it is mainly in Japanese).
Everyone should be a process owner
Dr. Iida wants each of the hospital employees to see MQI as their jobs – and that everyone sees themselves as a “process owner”.
I asked how they engage everyone as process owners. They shared that they are still working on it, and it is a challenge, but this is their goal. They also shared that it is hard to engage physicians in improvement work (I shared that this is not just a Japanese challenge!).
A challenge in healthcare

One challenge, they said, is that employees don’t “understand their job precisely” and they are unable to create a workflow chart of their work (which is part of the reason he wrote a book on how to create workflow charts).
I suggested that perhaps the inability to “understand their job precisely” is not solely because of a lack of knowledge of how to create a workflow chart.
In my experience of supporting improvement work in hospitals and health systems, it is rare that there are standard processes in the first place. When there is a high level of variation of the “same” process, it’s difficult to create a flow map of the workflow! The creation of standard work and stabilizing processes is a first (important) step in being able to improve.
So, I agree that knowledge of how to understand, to see, and to map a process is important. But we also need to strive for stable, reliable processes and create standard work so that employees can “understand their work precisely”.
Top take-aways
I am very appreciative of the time these two physician leaders gave to me and their passion for quality improvement. They are clearly committed to quality and to developing capability in others to be problem solvers.
My top three take aways from this gemba visit are:
- Leadership is critical – committed and dedicated leaders can change a culture and lead the way to improve
- Knowledge of how to improve is important – the tools and methodologies for improvement are essential
- Engaging everyone is a challenge – but when we do, we will see real transformation.
But most importantly – keep improving improvement
While I did not see some of the artifacts of “Lean” management that one might expect to see in a place like Toyota or other Japanese organizations with deep Lean practices (such as one I visited last year), or that exist in some U.S. and Australian healthcare organizations I’ve worked with – such as visibility boards linking policy deployment goals from senior leadership down to the local units – these leaders have created a culture of quality improvement. It isn’t about the tools or books, but rather the leadership approach to learning and improvement.
I will be interested in staying in touch with this hospital to see if and how they achieve in their goals – particularly of MQI squared – and what they learn along the way. It’s all about the process of improving the process of improvement itself.
How can they further engage everyone in improvement, and how might they continue to learn from Japanese industry and continue to evolve their approach to MQI?











